What are Perimenopausal Symptoms?
An Overview of the Symptoms of Perimenopause
The stage of life between a young woman’s fertility, and […]
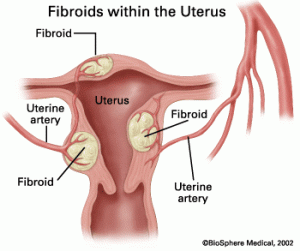 An Overview of Uterine Fibroid Treatment with Robotic Surgery
An Overview of Uterine Fibroid Treatment with Robotic SurgeryThe stage of life between a young woman’s fertility, and […]