Causes and Treatments of Female Urinary Incontinence
Female Urinary Incontinence Overview
An estimated 17 million women in the U.S. will cope with female bladder […]
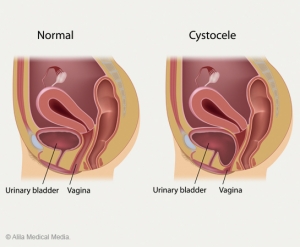 An Overview of a Prolapsed Bladder & Cystocele Repair Surgery
An Overview of a Prolapsed Bladder & Cystocele Repair SurgeryAn estimated 17 million women in the U.S. will cope with female bladder […]