What Are the Signs and Symptoms of Endometriosis?
An Overview of Endometriosis Symptoms
Endometriosis is a condition where endometrial tissue starts to grow outside of the uterus. Endometrial lesions […]
Can You Explain More About Uterine Fibroids?
An Overview of Uterine Fibroids
Many women living in the communities of Plano, Frisco and Dallas, Texas experience non-cancerous tumors in […]

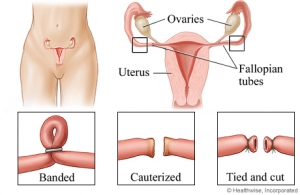 An Overview of Tubal Ligation Surgery as a Form of […]
An Overview of Tubal Ligation Surgery as a Form of […]