What is the Importance of an OBGYN?
 The Importance of OBGYN Specialists […]
The Importance of OBGYN Specialists […]
Is Tubal Ligation Surgery the Right Choice for Me?
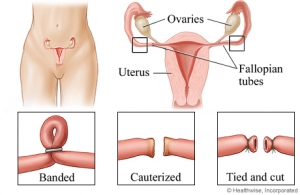 An Overview of Tubal Ligation Surgery as a Form of […]
An Overview of Tubal Ligation Surgery as a Form of […]
When is the Right Time to Start Going to the Gynecologist?
 An Overview of a Woman’s First OB Appointment
An Overview of a Woman’s First OB Appointment
When […]
2010 Medical Mission to Guatemala
Dr. Murray Fox, a Plano gynecologist, and Dr. Daryl Greebon, a Plano OBGYN, of Women’s Specialists of Plano […]
How Can I Stay Healthy During the Holiday Season?
Health During the Holidays Overview
Women need to make their health a priority and take care of […]
Endometrial Ablation as a Menorrhagia Treatment
 Dr. Jules Monier performs endometrial ablation […]
Dr. Jules Monier performs endometrial ablation […]
Can You Explain More About Uterine Fibroids?
An Overview of Uterine Fibroids
Many women living in the communities of Plano, Frisco and Dallas, Texas experience non-cancerous tumors in […]



 An Overview of a Woman’s First OB Appointment
An Overview of a Woman’s First OB Appointment